How Could I Not? My Experience Participating in a Clinical Research Study
I have been doing science for many years at the bench, with students, and in my kitchen, where I would study other organisms, cells, and molecules. But last fall, I spotted an opportunity to flip my relationship with science around and offer myself as part of someone else’s science experiment.
So far, I have been lucky to be quite healthy, which has driven me to help others when I can. I donate blood when I can, I am alerted of potential research studies by ResearchMatch.com, and I even felt disappointed when there was a new study related to my childbirth that didn’t work out for me to participate in.
But just this fall, an email popped into my inbox and I did meet all of their criteria:

How could I not offer myself as part of an experiment to help others?
I immediately replied with my phone number to get more information. After a straightforward conversation, I signed up and went in for a screening appointment.

Photography: Zach Veilleux
I got a detailed explanation of the research questions being studied. It turns out that many kids who had certain kinds of cancer were treated with abdominal or full-body radiation. As adults, many of these survivors lived “normal” lives and looked physically “normal” but were at elevated risks for many metabolic diseases related to obesity such as heart disease and diabetes. Many of them were fit, but still showed these risk factors. Scientists wanted to collect samples of their fat cells to see how it compares to un-radiated fat cells.
That’s where I came in: a source of un-radiated fat cells.
I was told what scientists would get out of it (hopefully lots of knowledge about fat metabolism) and what I would get out of it (nothing much). So, while I wouldn’t stand to gain much, and would be going through a somewhat-invasive fat biopsy procedure, I kept thinking about the childhood cancer survivors who wanted to live “normal” and healthy lives, and, I thought of the scientists asking big questions to better understand the human body. I felt fortunate to be able to help.
How could I not go through this procedure?
After the nurses did a basic exam and told me about the procedure, it looked like I would qualify as a participant in their study. Qualification was based on my health and how closely my body matched the characteristics of cancer-survivor patients in their study. This ensured I would be a meaningful control for these other characteristics (height, weight, sex, etc.). Finally, to schedule the actual study procedures, I had to go through an informed consent process. Although I was very familiar with this process (as a scientist and educator), I couldn’t help but notice the intention and gravity in the room as I was about to opt in to such a significant procedure.
To make sure I understood what I was agreeing to, the nurse practitioner, Jeanne, prompted me to explain the procedure in my own words:
Can you tell me what I’m going to do?
This is when it felt real.
Not only did I have to understand (on some level) what would happen, but feeling the words move through my mouth foreshadowed the feeling of the biopsy on my abdomen. As a scientist, the words weren’t that foreign for me, but still the idea of talking about them in the context of myself was an entirely new experience. As an educator, the power of this question for demonstrating true informed consent was not lost on me—saying it aloud solidified my understanding and my acknowledgement, just as the saying goes “you don’t know it until you teach it.” This was my mini teach-back session.
Naturally, after this I was both curious to see what the body fat assessment and biopsy would actually be like and nervous about whether the risk and the steps involved were worth it. In moments of doubt, I caught myself thinking, “why subject myself to these tests unnecessarily?”.
After completing this screening and lots of paperwork, I was scheduled for my procedures in about two weeks….
—-
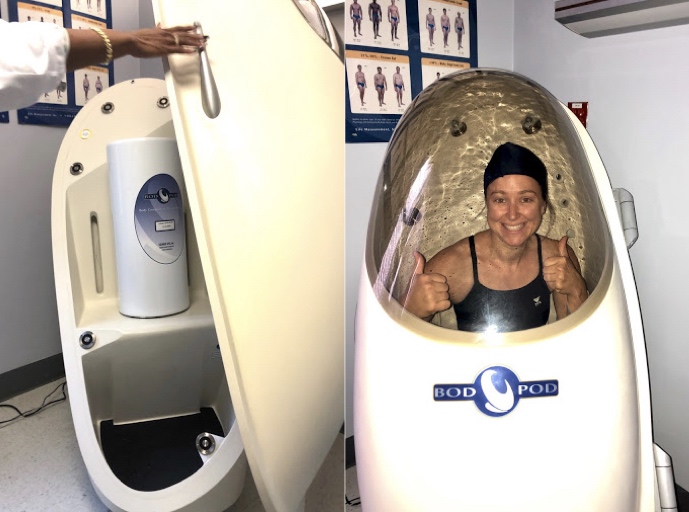
Disan Davis settles into the BodPod as part of the research study.
On a Wednesday morning in October, 2019, I began my day with my usual routine, but refrained from eating breakfast. I had to arrive having fasted for the past 12-hours (luckily I was asleep for most of them!). When I arrived at the hospital, I was greeted by the front desk staff, the nurses I had met on my first visit, and a slew of nursing students whom I had allowed to observe the procedure.
I was whisked off with hospital personnel through a quiet hallway that felt like a deserted hospital wing for the first part of my assessment: the fat analysis test in the BodPod! This was an extremely brief adventure in a spaceship-shaped device carefully designed to measure body fat percentages using displaced air (to measure volume) relative to one’s current weight. To be most accurate, I was asked to wear tight-fitting clothes, hence the bathing suit. While I was warned that the BodPod could feel claustrophobic and given repeated reminders that I could stop at any time—this was yet another nod to the informed consent process that was woven throughout my experience—, it was a quick and painless process for me.
 Then, onto the major test of the day, the fat biopsy. Jeanne again asked the big question: “Can you tell me what I’m going to do?” and I had to describe my understanding of the procedure. I was still offered the option to end my participation in the study—ensuring that this was voluntary and intentional—but I was in it for the long haul.
Then, onto the major test of the day, the fat biopsy. Jeanne again asked the big question: “Can you tell me what I’m going to do?” and I had to describe my understanding of the procedure. I was still offered the option to end my participation in the study—ensuring that this was voluntary and intentional—but I was in it for the long haul.
A nurse came in to draw my blood and help me to get set up. In addition to Jeanne, the nurse practitioner preparing and performing the fat biopsy, I was surrounded by nursing students and an assistant.. As I laid on the table, prepping as one would for any sterile surgery environment, I became, again, acutely aware of the gravity of the procedure. But, I was also curious and felt overwhelmingly lucky for my good health.
How could I not go through this procedure?
 The procedure lasted 15 minutes, timed on a large wall clock, and produced 3g of fat for the research laboratory. The process is identical to liposuction, though to lose a noticeable amount of fat I would have laid there for hours.
The procedure lasted 15 minutes, timed on a large wall clock, and produced 3g of fat for the research laboratory. The process is identical to liposuction, though to lose a noticeable amount of fat I would have laid there for hours.
 Afterward, I was taped shut with a very small butterfly bandage and given breakfast in my recovery room. The egg sandwich and coffee were much appreciated since I had been fasting for 12 hours and at this point I was really hungry! I was checked on and my coffee was refilled, so I was well taken care of in my brief recovery period.
Afterward, I was taped shut with a very small butterfly bandage and given breakfast in my recovery room. The egg sandwich and coffee were much appreciated since I had been fasting for 12 hours and at this point I was really hungry! I was checked on and my coffee was refilled, so I was well taken care of in my brief recovery period.
Meanwhile, my blood draw and fat biopsy samples were whisked off by a laboratory scientist for her to prepare and freeze for future study.
––
After just a couple weeks, my incision was marked only by the smallest scab, not much bigger than a pin prick. I am fully healed and back to the bustle of everyday life, hardly thinking about this moment. But when I do, I remember how my cells are now in a freezer at Rockefeller University, with some promise of helping to better understand fat metabolism and the effects of radiation.
Who knows what my tiny cells can do—how could I not be a part of something so big?
